This website uses cookies so that we can provide you with the best user experience possible. Cookie information is stored in your browser and performs functions such as recognising you when you return to our website and helping our team to understand which sections of the website you find most interesting and useful.
What is Primary Open-Angle Glaucoma (POAG)?
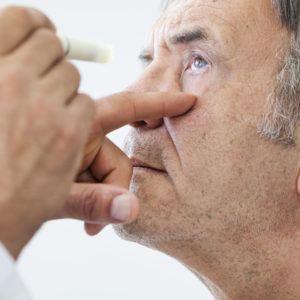
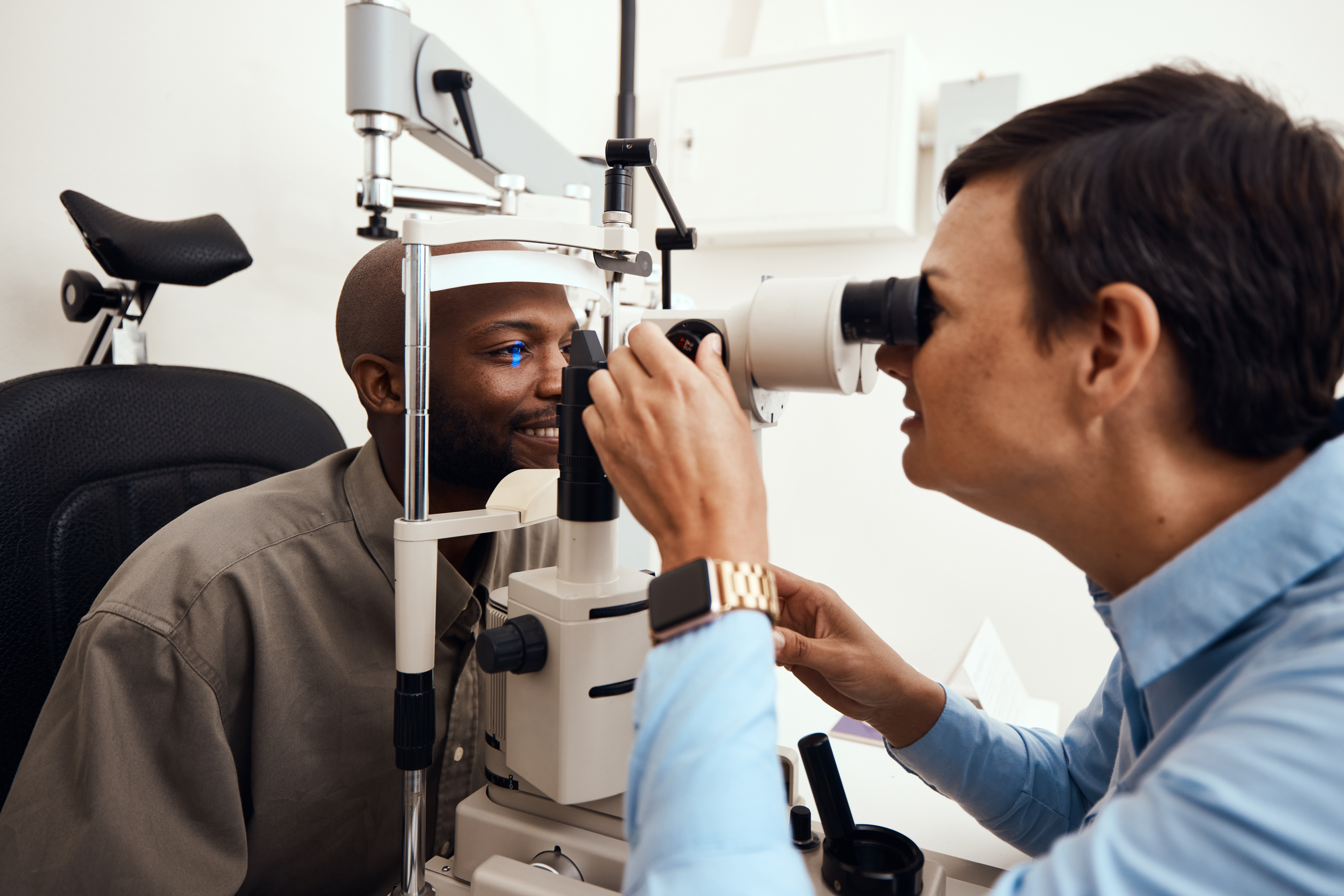
Primary open-angle glaucoma is the most common form of glaucoma, and is a disease of the optic nerve in the back of the eye, where “cupping” of the optic disc occurs, caused by increased pressure inside of the eye. Glaucoma is the 2nd leading cause of blindness globally and patients usually do not experience symptoms until more advanced visual field defects are seen. Vision loss due to glaucoma cannot be reversed.1
Signs & Symptoms
- Increased pressure in the eye
-
Blindness beginning with outermost vision that tunnels inward
Important Note on POAG
Increased pressure inside the eye puts stress on the optic nerve and causes irreversible blindness. Glaucoma is considered a silently blinding disease because it targets our outermost vision first and then tunnels inward. Therefore, it’s extremely important to maintain comprehensive eye exams and follow-ups as recommended by your primary eye care provider.
“Understanding Glaucoma” by Sharp HealthCare