Ora, Inc websites use cookies. By continuing to browse the site you are agreeing to our use of cookies. For more details about cookies and their use, please see our Privacy Policy.
What is Dry Eye?
Dry eye is a disease of the front of the eye, whereas a disruption in our normal tear production and maintenance occurs.1 There are two main types of dry eye: aqueous deficient dry eye and evaporative dry eye.
Aqueous deficient dry eye occurs when too little tears are produced by the lacrimal gland located below our eyebrow.3 When we don’t have adequate aqueous tear production, our ocular surface becomes rough, causing burning, gritty, and scratchy eyes. Wearing contact lenses or having a history of previous eye surgery can contribute to this type of dry eye.4
Evaporative dry eye, also known as meibomian gland dysfunction (MGD), stems from the clogging of the meibomian glands inside of our eyelids. Our meibomian glands secrete meibum, the lipid or oily layer of the tear film. This tear layer helps to keep the other layers of the tear film in place. When our meibomian glands are clogged, our tears can evaporate easily, causing irritation.5
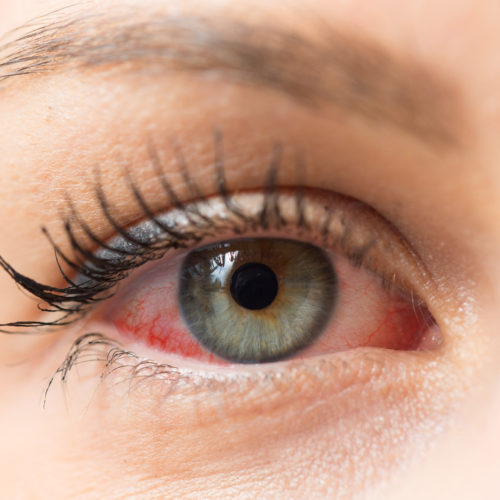
Signs & Symptoms
- Redness
- Watering
- Burning
- Blurry vision
- Decreased tolerance and discomfort when wearing contact lenses.11
“Dry eye: symptoms, causes and treatments” by EyeSmart – American Academy of Ophthalmology